During a recent shift, emergency physician Amanda Bates at the Mount Sinai health system in New York City, USA, had to put six patients on ventilators and transfer them to the intensive care unit.
`Before deciding to intubate, I always try to call the patient’s family if possible. But recently many patients are in such critical condition that I don’t have time to do that anymore,`
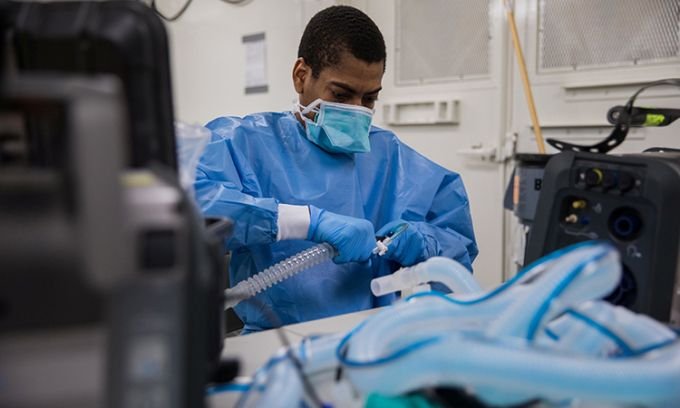
A technician installs a ventilator at Javits Medical Center in New York City.
The US has recorded more than 435,000 infected people and nearly 15,000 deaths from nCoV.
As the number of infections continued to increase sharply, including many critical cases, many hospitals in New York City had to prepare the worst scenarios about having to choose `who to let go and who to save`.
Several hospitals and New York state health department leaders have issued guidance on criteria for placing patients on ventilators in the event hospitals run out of the medical equipment.
Northwell Health, a medical system with 23 member hospitals, plans to prioritize ventilators for patients with the highest likelihood of survival, based on a scoring system issued by New York state officials in 2015. Scores
Northwell leaders are having difficulty choosing between patients with equal scores.
`We don’t advocate taking it as a game of chance. We want every patient to be treated fairly,` said Renee McLeod-Sordjan, director of medical ethics for the Northwell system.
Northwell only has about a quarter of its reserve ventilators left and 88% of beds in intensive care units are full of patients.
Mount Sinai health system leaders recently sent a directive to doctors in six emergency departments that ventilators would not be available to patients with no chance of survival, such as those in cardiac arrest or who do not meet the criteria for survival.
Brendan Carr, chief of emergency medicine at the Icahn School of Medicine at Mount Sinai, said the guidance serves as a reminder about making the best choice.
Mount Sinai is also teaching emergency physicians how to respond to difficult questions from families of patients who want to prolong treatment.
`I wish things could be different. These are unusual times. Your grandmother’s health condition does not meet the criteria for admission to the ICU today,` the script said, stating how the doctor would respond.

A patient was transported to Wyckoff Heights Medical Center, Brooklyn County, New York City.
Sean Morrison, chief of geriatrics and palliative care at the Icahn School of Medicine, said the guidance is intended for when hospitals face a `worst-case scenario` of medical equipment shortages and have
According to health officials, such preparations are necessary to deal with the Covid-19 crisis and the current ever-increasing number of cases in New York City.
Governor Andrew Cuomo said earlier this week that the Covid-19 crisis in the state may be peaking and pressure on hospitals is easing thanks to the arrival of 1,000 ventilators from China and hundreds from other US states.
State health leaders are updating guidance from 2015 to help hospitals have a way to distribute ventilators in case they run out of stock.
`People who are forced to make difficult choices know that no matter what they do, the outcome will be terrible. Therefore, it is better if they are not under pressure to
However, the final version of the new guidelines has not yet been published.
New York lawmakers recently passed a measure to protect health care workers and hospitals in medical malpractice lawsuits while the health system is overwhelmed by Covid-19.

Field hospital in New York Central Park.
Robert Femia, chief of emergency medicine at NYU Langone Hospital, told doctors in an email last month to `be more thoughtful` about patients requiring ventilators.
Until now, NewYork-Presbyterian Hospital has been using available medical ethics guidelines to determine when `hopeless patients` should be taken off the ventilator, according to chief executive officer Steven Corwin.
`Patients on ventilators who have permanent organ failure or lung failure are the ones we will take off life support. That rule applies even without a pandemic, but it has been upgraded,`
Dr. Corwin said NewYork-Presbyterian will not formulate a policy that completely follows the state’s guidance from 2015, saying the patient scoring system remains flawed.
Calculating a survival score based on factors such as age, chronic disease and organ failure is not a best practice and cannot replace clinical assessment and discussion between the patient’s family and the treating physician.
Art Fougner, president of the New York State Medical Association, said health officials should avoid putting a doctor under pressure when forced to choose which patients should die.